The group aims to vaccinate about 20% of the people in the world, focusing on hard-to-reach populations in Africa, Latin America, and Asia. To do so, it needs another $4.9 billion in addition to the $2.1 billion it has already raised. But there are other problems. The cheaper and easier-to-transport vaccines like the ones pledged by AstraZeneca have been slower to gain regulatory approval. Meanwhile, other companies seem less interested in pitching in: Doctors Without Borders found that only 2% of Pfizer’s global supply had been granted to Covax, and Moderna is still “in talks” with the organization.
“Covax is a critical starting point that—without a commitment from President Biden—had a high probability of failure. It’s looking better now, but could still fail if it doesn’t get money and vaccines,” says Barry Bloom, a global health researcher at the Harvard T.H. Chan School of Public Health. Biden officially directed the US government to join Covax in late January.
If it can succeed, the international program has many upsides. It establishes a mechanism of fairness that doesn’t depend on colonial mentalities of quid pro quo, says Bloom. It also absolves individual rich countries from having to determine which countries get what percentage of the vaccines. “This is a way of saying somebody else will take the rap, especially for the delivery time,” he says.
We’re not safe until we’re all safe
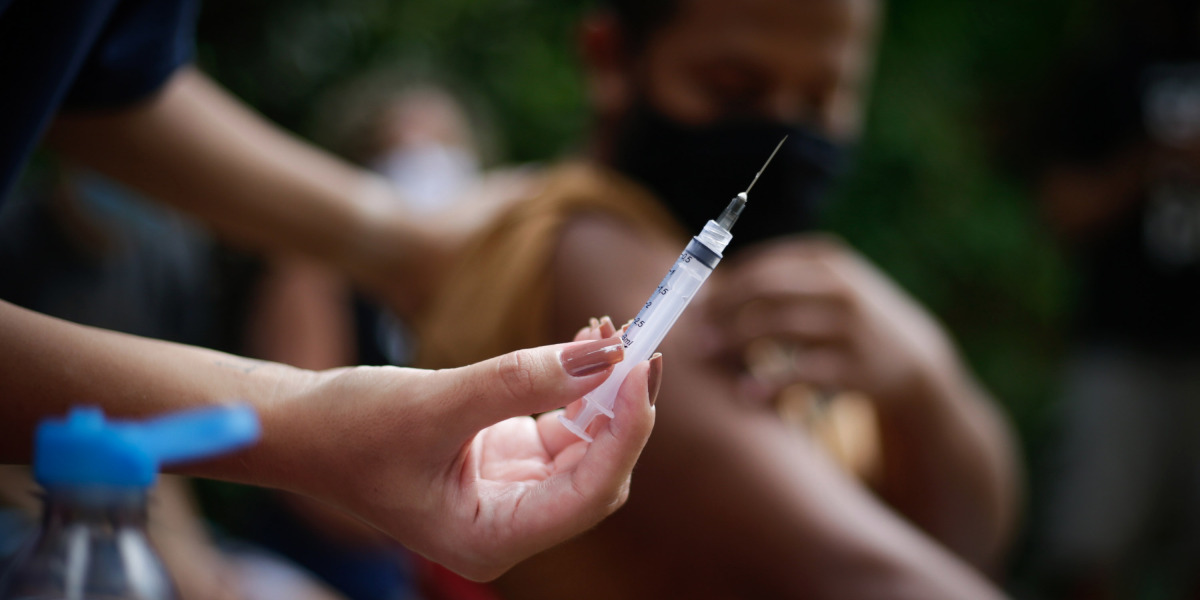
The motive for getting the vaccine to poorer countries more quickly is not just altruism: evolution will punish any delays. SARS-CoV-2 has already mutated into several worrying new variants, and this process will continue. If countries with large populations wait to be vaccinated for years, the virus will keep mutating—potentially to the point that the first available vaccines lose effectiveness. That will be bad for everyone, but poorer countries, with less access to updated vaccines, will again feel more of the impact.
“We get more mutants and they get more deaths,” says Bloom.
Judd Walson, a global health researcher at the University of Washington, worries more about the indirect effects of the pandemic in the developing world, where in many places covid-19 doesn’t even rank in the top 20 causes of death. Health systems have directed a lot of personnel and resources to dealing with the pandemic—setting up quarantine centers, doing surveillance, and more. In addition, funders and ministries have been diverted away from diarrhea, malaria, and other killers.
As a result, those other programs are suffering: rates of immunization for diseases such as measles, diphtheria, tetanus, and whooping cough are declining, both for lack of supplies and personnel and because people fear going to health centers. “All those other things that are killing people are being neglected, so not providing a covid vaccine stops governments from shifting back to their priorities before the pandemic,” says Walson.
And while virus variants can travel fast in a highly connected world, so can economic instability. That’s one takeaway from a recent paper published by the nonprofit National Bureau of Economic Research. Sebnem Kalemli-Özcan, an economist at the University of Maryland, and colleagues analyzed how delays in global vaccine distribution would affect the economies in countries whose populations had already been vaccinated.
The economic cost of inequity
They found that a world where poorer countries have to wait to be vaccinated would see a global economic loss of about $9 trillion this year, with wealthy countries absorbing nearly half of those losses in declining trade and fractured supply lines. (A similar study by the RAND Corporation estimated that failure to ensure equitable covid-19 vaccine distribution could cost the global economy up to $1.2 trillion a year.) Ensuring equitable distribution is actually in the best interests of advanced economies. “Their hit will come back and hit you,” says Kalemli-Özcan.